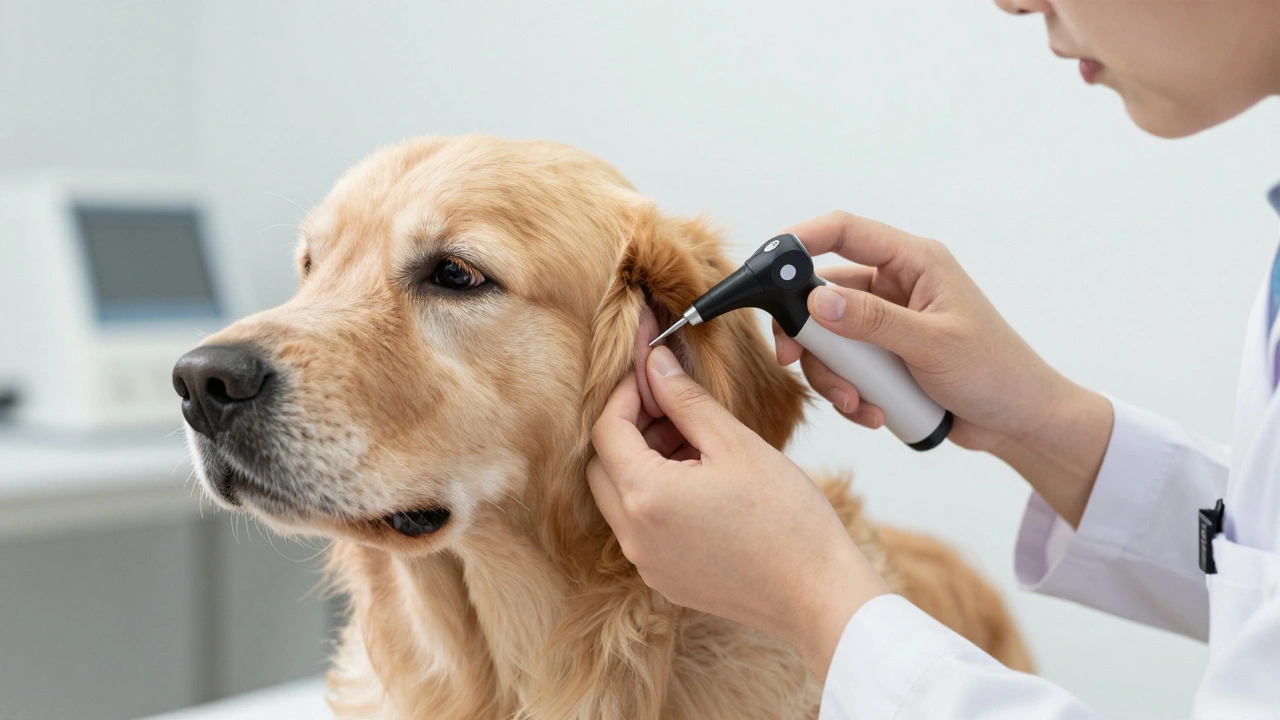
When your dog shakes their head like a windshield wiper or scratches at their ears until they bleed, you know something is wrong. But the real story isn't just on the surface. It’s inside the canal, hidden from plain sight. That’s where otoscopy comes in. This diagnostic procedure is the gold standard for identifying what’s actually happening in your dog's ear, especially when infections have lingered for months or years.
In chronic cases, the damage often goes deeper than simple redness or discharge. The structures of the ear can change shape, narrow, or close up entirely. Without looking directly inside with an otoscope-a handheld device with a light and magnifying lens-vets are essentially guessing. And guessing leads to treatments that fail, leaving your pet uncomfortable and frustrated.
The Anatomy of a Problem Ear
To understand what vets see during an otoscopic examination, you first need to visualize the dog’s ear anatomy. Unlike humans, dogs have L-shaped ear canals. The vertical part runs down into the skull, while the horizontal part extends toward the eardrum (tympanic membrane). This shape makes drainage difficult and traps moisture, debris, and bacteria.
In healthy dogs, this canal is pink, clean, and open. In chronic cases, however, the tissue reacts to long-term inflammation. The skin thickens, glands overproduce wax, and hair follicles may grow excessively inside the canal. Over time, these changes create a perfect environment for pathogens to thrive. Common culprits include yeast (Malassezia pachydermatis), bacteria like Staphylococcus pseudintermedius, and even ear mites, though mites are less common in older dogs with established issues.
The goal of otoscopy isn’t just to spot dirt. It’s to assess the integrity of the entire canal system. If the canal has narrowed due to scarring-a condition called stenosis-topical medications won’t reach the source of the infection. Similarly, if the eardrum is ruptured, certain drops could cause severe pain or hearing loss by entering the middle ear space.
What Vets Look For During Otoscopy
During the exam, the veterinarian inserts the otoscope tip gently into the ear canal. They rotate the instrument to get a full view of the vertical and horizontal segments. Here’s what they’re scanning for:
- Discharge Type: Is it clear, bloody, pus-like, or foul-smelling? Yeast infections typically produce a brown, coffee-ground-like discharge. Bacterial infections might yield yellow-green pus.
- Skin Changes: Thickened, darkened, or ulcerated skin suggests long-standing inflammation. Healthy pinnae (ear flaps) should be thin and flexible; stiff or rigid ears indicate fibrosis.
- Eardrum Status: A bulging, opaque, or absent tympanic membrane signals rupture or fluid buildup behind it. Ruptures are serious because they connect the outer ear to the inner ear, risking balance disorders and deafness.
- Polyps or Growths: Benign polyps or malignant tumors can obstruct the canal. These appear as fleshy masses protruding from the canal wall or near the eardrum.
- Foreign Bodies: Grass awns (“foxtails”), splinters, or other debris lodged deep in the canal require immediate removal to prevent abscess formation.
If any of these signs are present, the vet will likely take samples for cytology (microscopic analysis) and culture (bacterial growth testing). Cytology reveals whether yeast, bacteria, or both are dominant. Culture identifies specific strains and their antibiotic sensitivities, guiding targeted treatment.
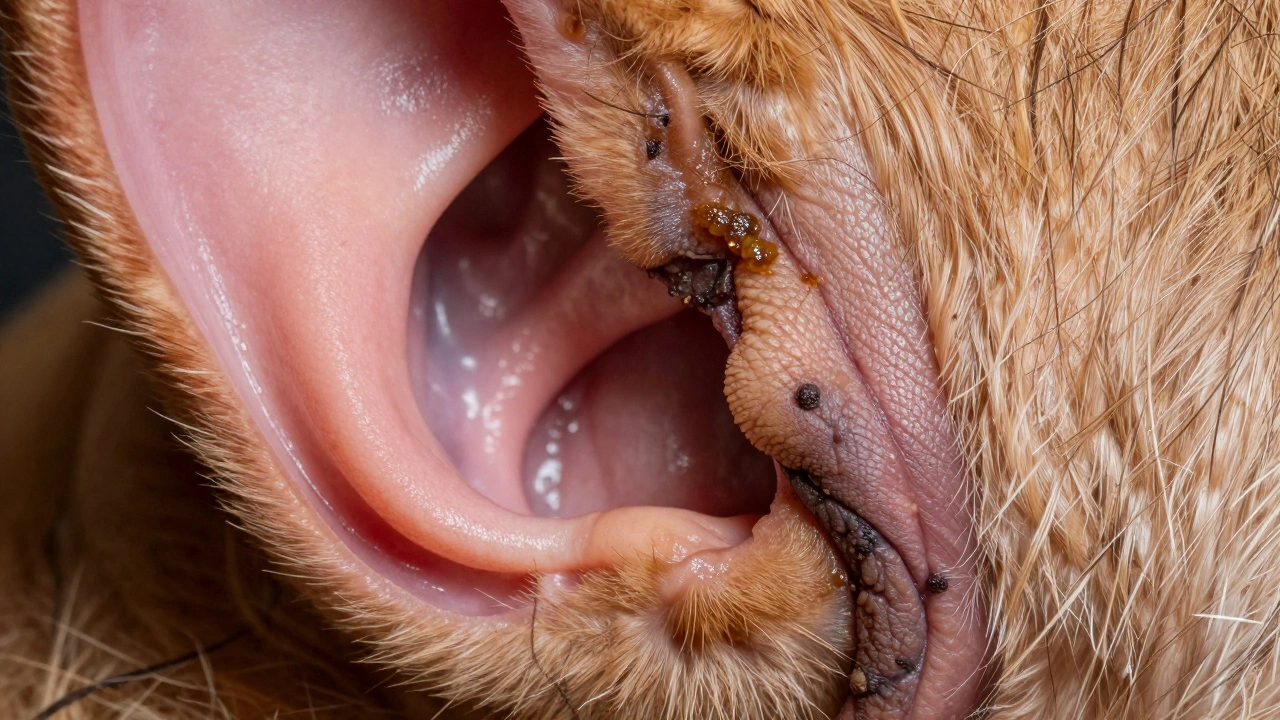
Chronic vs. Acute: Why Duration Matters
An acute ear infection develops suddenly and usually responds well to short-course therapy. Chronic ear disease persists beyond three months despite treatment. At this stage, the ear’s architecture has changed permanently unless surgically corrected.
Consider this scenario: Your dog had recurrent ear infections treated with steroid drops every few weeks for two years. Each flare-up caused temporary relief but allowed underlying inflammation to worsen. Now, the canal walls have become so thickened that medication cannot penetrate effectively. Even if you clean the ear daily, the trapped debris continues to feed microbes.
This is why duration matters. Long-term exposure to irritants triggers adaptive responses in the body. Cells multiply rapidly to repair damage, leading to hyperplasia (excessive cell growth). Blood vessels dilate constantly, causing persistent redness. Nerve endings become hypersensitive, resulting in chronic pain even without active infection.
Vets classify chronic ear disease based on severity:
- Mild: Minimal stenosis, intact eardrum, mild inflammation.
- Moderate: Partial stenosis, possible small perforation, moderate swelling.
- Severe: Near-complete occlusion, large rupture, extensive scar tissue.
Classification determines whether medical management suffices or surgery becomes necessary.
Tools Beyond the Otoscope
While otoscopy provides visual confirmation, additional tools help paint a complete picture. Many clinics now use video otoscopes connected to monitors, allowing owners to see exactly what the vet sees. Some advanced practices employ endoscopic cameras capable of navigating tight spaces within the canal.
For suspected middle ear involvement, imaging studies such as X-rays, CT scans, or MRIs may be recommended. These reveal soft tissue abnormalities invisible through direct visualization alone. Fluid accumulation, bone erosion, or mass lesions behind the eardrum show up clearly on cross-sectional images.
Allergy testing also plays a role since food allergies and environmental allergens contribute significantly to chronic ear problems. Identifying triggers helps reduce recurrence rates after initial treatment.
| Method | Purpose | Limitations | Best Used When... |
|---|---|---|---|
| Otoscopy | Visual inspection of ear canal and eardrum | Limited depth penetration; requires cooperation | Initial assessment of visible pathology |
| Cytology | Identify microbial types under microscope | Does not identify species-level bacteria | Determining primary cause of inflammation |
| Bacterial Culture | Pinpoint exact bacterial strain and sensitivity | Takes 48-72 hours; costlier | Recurrent or resistant infections |
| Imaging (CT/MRI) | Evaluate middle/inner ear structures | Expensive; often requires anesthesia | Suspected tumor or structural anomaly |
Treatment Strategies Based on Findings
Once the vet understands what’s going on inside the ear, they tailor treatment accordingly. Mild cases respond well to medicated cleansers followed by topical antibiotics or antifungals. Moderate cases might need oral steroids to shrink swollen tissues before applying drops.
But here’s the catch: if the canal is severely stenotic or the eardrum is ruptured, conventional medicine fails. In those situations, surgical intervention becomes unavoidable. Procedures range from partial ablation (removing diseased tissue) to total ear canal resection (TECA), which eliminates the external ear canal altogether.
TECA sounds drastic, but it offers permanent relief for dogs suffering from debilitating chronic otitis. Post-surgery, most patients experience improved quality of life, fewer vet visits, and reduced dependency on expensive medications.
Another option gaining popularity is laser-assisted ablation. Using precise beams of light, surgeons vaporize abnormal tissue while preserving surrounding healthy areas. Recovery times are shorter compared to traditional methods, making it attractive for elderly or frail patients.
Preventing Future Flare-Ups
Even after successful treatment, maintaining ear health remains crucial. Regular cleaning using pH-balanced solutions prevents buildup of cerumen (wax) and moisture. Avoid cotton swabs-they push debris deeper and risk damaging delicate tissues.
Trimming excess hair around the entrance to the ear improves airflow and reduces humidity levels. For breeds prone to floppy ears (like Spaniels or Retrievers), keeping them upright occasionally allows natural drying.
Dietary adjustments matter too. Eliminating inflammatory foods rich in processed grains or artificial additives supports immune function. Omega-3 fatty acids found in fish oil promote healthier skin barriers, reducing susceptibility to secondary infections.
Finally, monitor closely for early warning signs: increased scratching, odor development, or sudden tilting of the head. Early detection means simpler interventions later.
How much does an otoscopy exam cost?
Prices vary depending on location and clinic type. Expect anywhere between $50 and $150 for basic otoscopy combined with physical examination. Additional tests like cytology ($30-$60) or culture ($75-$120) increase overall expenses.
Can I perform otoscopy at home?
Not safely. Consumer-grade otoscopes lack sufficient illumination and magnification needed for accurate diagnosis. Improper handling risks injuring the eardrum or pushing contaminants further inward. Leave professional evaluations to trained veterinarians.
Why do my dog’s ears smell bad?
Foul odors result from bacterial decomposition of organic material trapped inside the ear canal. Yeast produces sweetish mustiness, whereas anaerobic bacteria emit rotten egg-like stench. Persistent smells warrant prompt veterinary attention.
Is surgery painful for dogs?
Modern anesthetics ensure comfort throughout procedures. Pain management protocols include pre-operative analgesics, intraoperative nerve blocks, and post-operative NSAIDs. Most dogs recover smoothly within days to weeks.
Do all dogs need regular ear checks?
High-risk breeds-including those with hairy canals, pendulous ears, or history of allergies-benefit greatly from routine inspections. Low-risk individuals still deserve annual screenings during wellness exams.